The human uterine organ, especially the full-thickness endometria, is essential for fertilization and embryonic development. Human endometria, which mainly comprise endometrial epithelial and stromal cells, exhibit remarkable plasticity and undergo repeated injury and regeneration. The highly dynamic properties of repeated injury and scar-less repair during the menstrual cycle make it an ideal model to study tissue regeneration. Full-thickness injury or dysfunction of the human endometria causes intrauterine adhesion, miscarriage, and uterine factor infertility. The development of new regenerative technologies against intrauterine adhesion, miscarriage, and infertility diseases is hindered by our incomplete understanding of the molecular characterization of the cell populations responsible for scar-less endometrial regeneration during the menstrual cycle.
To help fill this knowledge gap, ZOU Xiaohui's research group from Zhejiang University published a research article entitled "SFRP4+stromal cell subpopulation with IGF1 signaling in human endometrial regulation" in Cell Discovery on September 27, 2022. The article identified the role and mechanism of SFRP4+ stromal cell subpopulation and its IGF1 signal pathway in promoting endometrial regeneration and repair, It provides a new therapeutic target for functional regeneration of endometrium.
First, this study used droplet-based single-cell RNA-seq (10x Genomics Chromium system) to profile single-cell suspensions from seven full-thickness normal human uterine tissues from two menstrual phases (3 from the proliferative-NP and 4 from secretory phase-NS). It identified main clusters as endometrial epithelia, stroma, endothelia, smooth muscle, and immune cells in the human uterus, and verified SFRP4+ stroma as proliferative phase-specific endometrial cell populations.
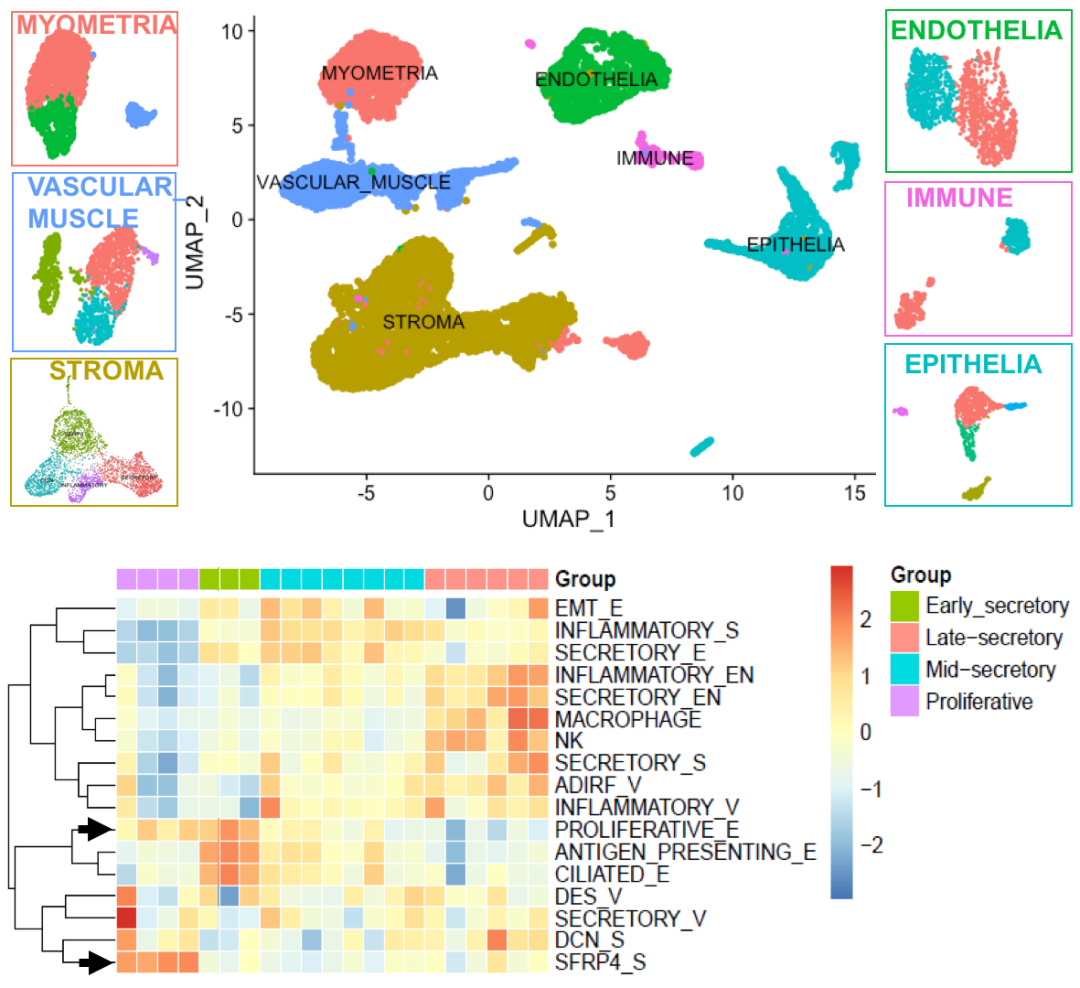
Fig. 1: Cell population architectures across the menstrual cycle identified SFRP4+ stroma cells as potential regenerative endometrial cell populations.
Next, the Connectivity analysis revealed IGF1 signals between SFRP4+ stroma cells and proliferative endometrial epithelial cells. Then they co-cultured SFRP4 + endometrial stromal cells with endometrial epithelial organoids, and confirmed SFRP4+ endometrial stromal cells promoting the proliferation of endometrial epithelial organoids in vitro through regenerative IGF1 signaling.
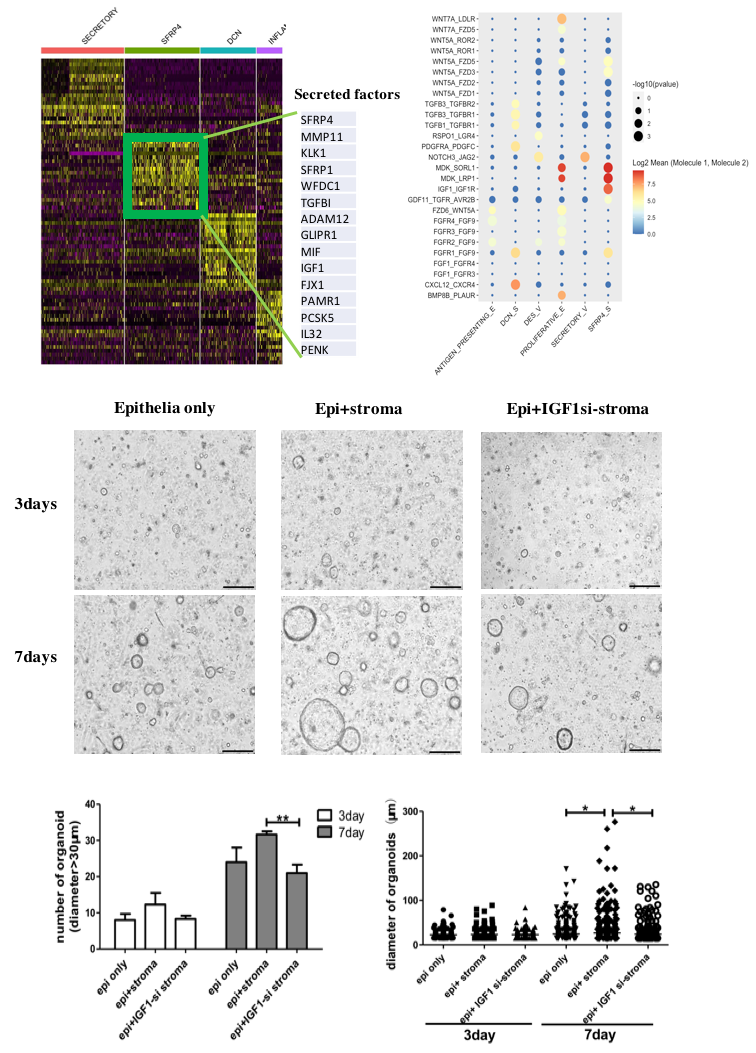
Fig. 2: SFRP4+ stromal cells promote the proliferation of endometrial epithelial organoid in vitro through regenerative IGF1 signaling.
At last, the study explored the regenerative potential of SFRP4+ endometrial stromal cells in an in vivo full-thickness endometrial injury model along with the effect of the key IGF1 signal molecule secreted from SFRP4+ stromal cells. A rat model of full-thickness endometrial injury was constructed. SFRP4+ endometrial stromal cells were mixed with gelatin methacryloyl (GelMA) hydrogel and transplanted into the injury site of the rat full-thickness endometrial injury model. The results showed that SFRP4 + stromal cells can promote the regeneration of endometrial epithelial glands and full-thickness endometrial injury through the IGF1 signaling pathway in vivo.

Fig. 3: SFRP4+ stromal cells promote the regeneration of endometrial epithelial glands and full thickness endometrial injury through IGF1 signaling pathway in vivo.
This study further sheds light on an SFRP4+ endometrial stromal cell subpopulation that is highly enriched in the regenerative stage of the endometria during the menstrual cycle. SFRP4+ stromal cells significantly enhanced the proliferation of endometrial epithelial organoids in vitro and promoted the regeneration of endometrial epithelial glands and full-thickness endometrial injury through the IGF1 signaling pathway in vivo. The cell atlas of full-thickness uterine tissues revealed the cellular and molecular mechanisms regulating the monthly regeneration of human endometria, which provides insights into the biology of human endometrial regeneration and the development of regenerative medicine treatments against endometrial damage and intrauterine adhesion.
The corresponding author of this article is Professor ZOU Xiaohui from the First Affiliated Hospital, Zhejiang University School of Medicine (FAHZU), the first author is Dr. WU Bingbing from the Fourth Affiliated Hospital, Zhejiang University School of Medicine, and the co-first author is Dr. Yu Li , Dr. Nanfang Nie and Xilin Shen from Zhejiang University School of Medicine. The research work was also strongly supported by professor OUYANG Hongwei from Zhejiang University School of Medicine, and the Department of Gynecology of FAHZU. This work was supported by the National Natural Science Foundation of China (81871127, 82171616, 31870973).


